In our first article in this series, we established the principle that the state in which you enter menopause determines how you experience it. A woman who arrives at this transition with a burdened gut, an overloaded liver, chronic stress, and years of unresolved emotional weight will have a fundamentally different experience than one who arrives with those systems in reasonable order.
This article is about two of those systems — the gut and the liver — and why, when they are struggling, menopause symptoms do not just worsen. They become relentless.
The Filter Analogy
Think of your gut and liver as a two-stage filtration system for your hormones. Used estrogen — estrogen that has already done its job — needs to be packaged, processed, and eliminated from the body. The liver packages it. The gut eliminates it through the stool. When both are working well, the process is clean and efficient. Hormone signals remain stable. The body knows what it has and what it does not.
Now imagine the filter is clogged.
A compromised gut does not eliminate used estrogen — it reactivates it. Enzymes produced by harmful gut bacteria break the packaging open, releasing processed estrogen back into circulation. Instead of leaving the body, it is recycled — like putting dirty water back through a broken filter and expecting it to come out clean. The result is chaotic, unstable estrogen signaling at precisely the moment when the body is already struggling to manage a hormonal transition.
The liver, meanwhile, is not just processing hormones. It is simultaneously managing toxins, medications, stress hormones, and the byproducts of chronic inflammation. During menopause, the demand on the liver increases — just as its capacity is often reduced by the very things that accompany modern life: poor sleep, chronic stress, and a diet that generates more waste than the system can efficiently clear.
The result is an overwhelmed body, juggling as much as it can to try to maintain balance.
The Root Causes — And the One Most People Miss
A compromised gut and an overloaded liver do not develop overnight. They are the accumulated result of years of choices and conditions — some dietary, some environmental, and some that run much deeper than what we eat.
Diet and lifestyle are the obvious contributors. A diet high in processed foods, sugar, and inflammatory fats feeds harmful bacteria and starves beneficial ones. Alcohol burdens the liver. Chronic sleep deprivation impairs both gut lining repair and liver detoxification. Medications, particularly antibiotics and anti-inflammatory drugs taken over years, alter the gut microbiome in ways that take significant time and effort to restore.
But there is a root cause that is rarely discussed with conventional doctors, and it is the one that explains why two women can follow the same gut protocol and get entirely different results.
These emotional states keep cortisol chronically elevated. Chronic cortisol elevation directly damages the gut lining, alters the microbiome, impairs liver detoxification, and locks the nervous system into the survival state that amplifies every menopausal symptom. The emotional fire and the physiological inflammation are not separate phenomena. They are the same fire, burning at two levels simultaneously.
This is why women who do everything right — the probiotics, the liver support, the anti-inflammatory diet — often find that the improvement plateaus, or that symptoms return when life becomes difficult again. The filter gets cleaned. But the fire that clogs it is still burning.
What a Struggling Gut Does to Your Hormones
When gut bacteria are out of balance — too much harmful bacteria, too little beneficial bacteria, an irritated or leaky gut lining — the consequences reach far beyond digestion.
Used estrogen that should be eliminated is reabsorbed. Hormone signals that should be stable become erratic. And the result, during menopause, is a cluster of symptoms that women often assume are simply part of the transition, but which are significantly amplified by gut dysfunction:
Hot flashes that are more frequent and intense than they should be. Mood swings that feel disproportionate. Anxiety that seems to arrive from nowhere. Headaches. Breast tenderness. Sleep that never fully restores. These are not just menopause. They are menopause on top of a gut that is feeding the fire instead of helping to put it out.
What an Overloaded Liver Feels Like
The liver is one of the most resilient organs in the body, and one of the most overlooked. It manages over 500 functions simultaneously, including the clearance of every hormone, toxin, medication, and inflammatory byproduct that passes through the bloodstream.
During menopause, as hormone metabolism shifts and the body's stress response becomes more reactive, the liver's workload increases. When it is already carrying years of accumulated burden — from a high-toxin environment, a nutrient-poor diet, chronic stress, disrupted sleep — it begins to fall behind.
The signs are not dramatic. They are quiet and persistent:
Fatigue that does not respond to rest. A vague sense of nausea or poor appetite. Headaches that come and go without clear cause. An increasing sensitivity to chemicals, perfumes, or alcohol. Weight that accumulates around the abdomen and resists every effort to shift it. A feeling that the body is simply not recovering the way it used to.
These are signs of an overwhelmed liver in need of support.
The Gut–Nervous System Connection
There is one more piece of this picture that explains why gut and liver dysfunction during menopause produces such a wide range of symptoms — including ones that seem to have nothing to do with digestion.
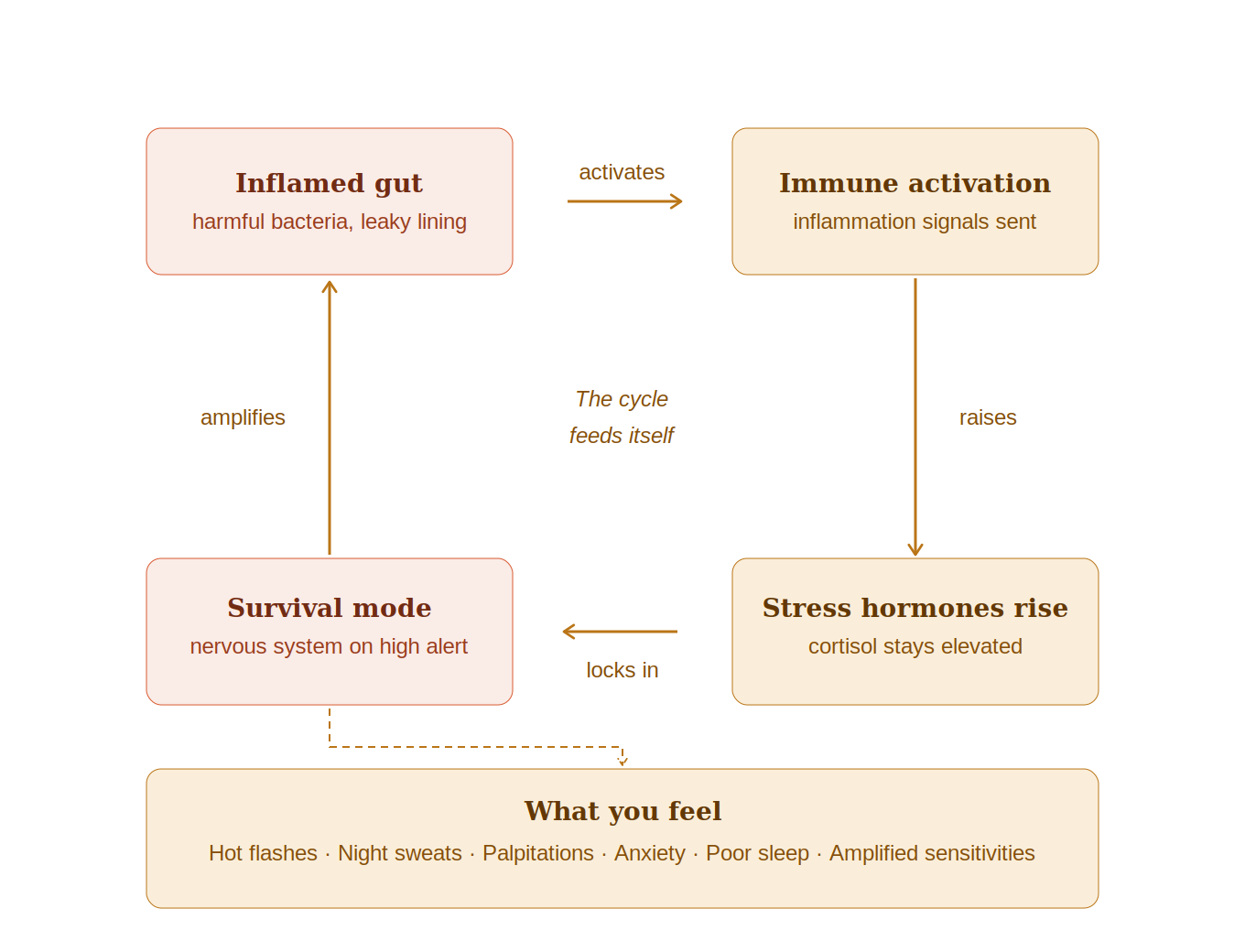
An inflamed gut activates the immune system. An activated immune system raises stress hormones. Elevated stress hormones lock the nervous system into survival mode. And a nervous system in survival mode amplifies every sensitivity the body has — heat, sound, emotion, physical sensation.
This is why gut dysfunction produces hot flashes, night sweats, palpitations, anxiety, and sleep disruption — symptoms that seem purely hormonal but are, in significant part, driven by a gut that is signaling danger to a nervous system that is already on high alert.
The gut and the nervous system speak to each other constantly. When the gut is inflamed, it tells the nervous system the body is under threat. The nervous system responds accordingly. And menopause, with its own hormonal turbulence, becomes the context in which all of this plays out at full volume.
Why Hormone Therapy Alone May Not Be Enough
Think of your hormonal system as a freeway. Hormones are the cars — they need to enter, travel, and exit efficiently through designated off-ramps. The liver and gut are those off-ramps. When they are functioning well, traffic flows. Hormones do their job and leave the system cleanly.
When the gut is inflamed and the liver overloaded, the off-ramps are blocked. Adding hormone therapy at this point — even the right hormones, carefully dosed — is like adding more cars to an already congested freeway with no working exits. The traffic does not move faster. It backs up. Bloating worsens. Headaches increase. Breast tenderness intensifies. Anxiety rises rather than settles.
The continuous symptoms do not indicate a failure of hormone therapy. They are a signal that the off-ramps need to be cleared first. You cannot expect smooth traffic flow when the exits are closed.
Cleaning the Filter — And Addressing the Fire
Physical support for the gut and liver makes a real difference. Calming gut inflammation through an anti-inflammatory diet — rich in fiber, fermented foods, colorful vegetables, and omega-3 fats — begins to shift the microbiome. Reducing the liver's burden by minimizing alcohol, ultra-processed foods, and unnecessary medications allows it to catch up. Stabilizing blood sugar prevents the cortisol spikes that feed both gut inflammation and nervous system reactivity. Restoring sleep gives the body the repair window it needs. And when the gut and liver are in better shape, hormonal support can work the way it was intended.
These are the right steps. They help. And they are necessary.
But they are not sufficient on their own — not for lasting change — because they address the consequences of the fire without addressing the fire itself.
Physical interventions clean the filter. But as long as the emotional fire burns, the filter will clog again.
Where True Healing Begins
This is the dimension of healing that no supplement can reach and no protocol can deliver — the dissolution of what is generating the problem at its source.
The women who experience the most complete and lasting recovery from the symptoms described in this article are not necessarily those who follow the most rigorous physical protocols. They are the women who do the inner work alongside the physical work. Who address the fear, the unforgiveness, and the unresolved emotional burden not through years of therapy that processes without releasing, but through a genuine reconnection to the spirit and to the healing Power of the Creator.
The spirit, when reconnected to Divine Power, carries a calming and restorative force that reaches places cortisol cannot. It does not manage the stress response. It dissolves what is generating it. It is the only water that can put out the fire for good.